Have any questions?
+44 1234 567 890


Director International Office
Prof. Dr. med. Sebastian von Peter
Tel: +493363883501
Mail: international@mhb-fontane.de
Incoming – Studies at the MHB
We are pleased to learn that you are interested in performing part of your studies or a complete course of studies at the Brandenburg Medical School. For any questions in this context please contact the International Office.
Medicine
What the Brandenburg Medical School stands for is a concept of medicine by humans for humans. Our students are supposed to acquire not only science-based medical knowledge but in addition all competences and skills required for medical doctors. Our study course of medicine is a model curriculum.
The standard period of studies in the medical curriculum at the Brandenburg Medical School including the exam period for the third part of the medical examination is six years and three months (§ 1 para 2 ÄApprO - regulations for the licensing of medical doctors).
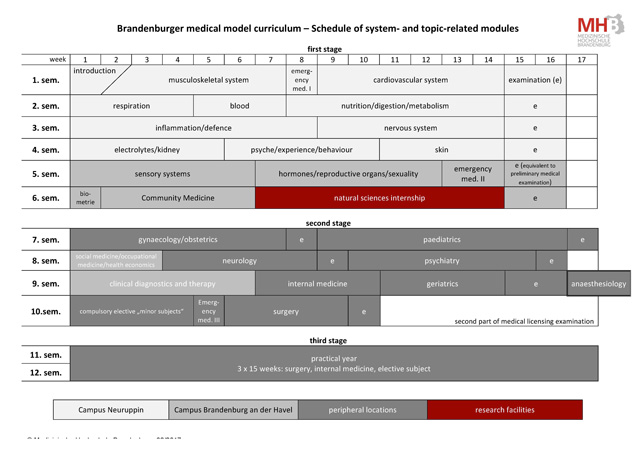
The programme is divided into three sections. Contents of the first part (1st sem. up to and including 6th sem.) cover body organs and systems. Building on this, the second part of the programme (7th sem. up to and including 10th sem.) addresses typical phenomena from various stages in life and various disciplines. The third part (11th and 12th sem.) is the Practical Year.
Pursuant to licensing regulations for medical doctors governing medical training in the Practical Year (§ 3 ÄApprO), students complete three internships of sixteen weeks respectively during the Practical Year. The programme concludes with the third section of the medical examination pursuant to licensing regulations for medical doctors.
Im course catalogue offers detailed information on modules. More information is available from the Section Curricular Development and Coordination.
Psychologie
The degree programme of Psychology focusses on a holistic perspective of human perception, experience and behaviour and combines the conveyance of a broad basis of knowledge in psychology with practical work in the field of clinical psychology and psychotherapy. The programme is organised in the form of a Bachelor course (B.Sc.) and a Master course (M.Sc.).
Semesters abroad
We are pleased to learn that you are interested in spending one or more semesters at the MHB. Please ensure that you are informed about the programme organisation, and let us know which subject-related semester(s) you wish to spend at the MHB.
General information
Please note that the MHB charges tuition fees. These are 12.500€ (medicine), resp. 4.980€ (Bachelor psychology) and 4.110€ (Master psychology) per semester. If you plan an exchange semester with Erasmus+, you will only pay tuition fees at your home university. For more information on MHB programmes see here.
German language skills
The language of instruction at the MHB is German. Pertinent language qualifications are essential for admission. We would recommend at least level B2 (Common European Framework of Reference for Languages).
Application
As a first step, please contact your home university and establish requirements for a study period abroad. As soon as you get permission from your home university, please contact the MHB International Office so that we can jointly plan the next moves. This is also possible if no partnerships or exchange agreements between the MHB and your home institution have been established so far.
Application period
The academic year at the MHB comprises two semesters, so that you may apply for a start in the winter or summer term. Please note the semester-specific module contents. The deadline for applications to be submitted to our International Office is at least one year prior to the start of the respective semester.
Application documents
Please submit the following application documents:
-
application form
-
curriculum vitae without photo
-
copy of current certificate of enrolment issued by home university
-
proof of German language skills
-
proof of overseas health insurance
-
copy of passport (for non-EU nationals)
-
evidence of vaccination status (only for medical students)
-
description of modules already completed
-
letter of motivation (2 pages max.)
-
Transcript of Records
Please send your complete application documents to international@mhb-fontane.de.