Have any questions?
+44 1234 567 890
Medizin studieren
Studiere deinen Traum.
Ohne NC, staatlich anerkannt, praktisch praxisnah.
Vorteile des Medizinstudiums an der MHB
Staatlich anerkannt, aber kein NC
Hohe Abschluss- und Bestehensquote in Regelstudienzeit
Moderne Lern- und Prüfungsformate
Praxis und Patient:innen von Beginn an
Kleine Lerngruppen
3 Universitätskliniken im Verbund an vier Standorten
Großes Netzwerk an kooperierenden Kliniken und Praxen
Promotion zum Dr. med. in allen Bereichen medizinischer Forschung
Stipendien und attraktive Finanzierungsmöglichkeiten
Modellstudiengang
Der staatlich anerkannte Brandenburgische Modellstudiengang Medizin (BMM) steht für praxisorientierte und wissenschaftsbasierte Lehrkonzepte sowie für die Einheit von Forschung, Lehre und Patient*innenversorgung. Das Medizinstudium an der MHB orientiert sich im hohen Maße an der klinischen Praxis und an Patient*innen und verfolgt das Ziel, die Studierenden fachlich und persönlich optimal auf die Herausforderungen ihres Berufes vorzubereiten.
Sowohl im individuellen Auswahlverfahren als auch im praxisorientierten Studium spielen Persönlichkeit und Persönlichkeitsentwicklung eine zentrale Rolle. Die Auswahl der Studierenden erfolgt dabei nicht nach einem notenbasierten NC, sondern nach persönlicher Eignung und beruflicher Vorerfahrung. In unserem Auswahlverfahren legen wir dementsprechend einen großen Wert auf Motivation und bisherige Erfahrungen.
Was uns auszeichnet
Ein Medizinstudium an der MHB unterscheidet sich in folgenden wesentlichen Punkten von dem an anderen Hochschulen:
-
Die MHB verfügt über ein Universitätsklinikum im Verbund und ermöglicht ihren Studierenden damit ein Studium auf höchstem medizinischen und akademischen Niveau, bei dem natürlich auch eine Promotion möglich ist.
-
Die Trennung in Vorklinik und Klinik im konventionellen Regelstudiengang ist im innovativen Brandenburger Modellstudiengang Medizin zugunsten eines integrierten und praxisorientierten Curriculums aufgehoben. Für die Studierenden hat das den Vorteil, dass die theoretischen Grundlagen in Biologie, Chemie und Physik immer auf die klinische Praxis und den individuellen Fall bezogen werden, wodurch das Lernen zwar immer noch anspruchsvoll bleibt, aber insgesamt sehr viel leichter fällt als in herkömmlichen Regelstudiengängen.
-
Wie in anderen Modellstudiengängen gibt es auch im Brandenburger Modellstudiengang Medizin keine Trennung zwischen Vorklinik und Klinik, dementsprechend gibt es auch kein separates "Physikum". Die sogenannte M1-Prüfung wird integriert als M1-Äquivalent absolviert.
-
Anders als bei medizinischen Hochschulen mit Regelstudiengang ist das Risiko, an dieser Hürde zu scheitern, nicht sehr groß. Zumindest wurde bislang von allen Studierenden der MHB das M1-Äquivalent ohne Verzögerung bestanden, was auch mit ein Grund dafür ist, dass die Abschluss- und Bestehensquote in Regelstudienzeit an der MHB herausragend hoch ist.
-
Es gibt vom ersten Semester an einen hohen Praxisanteil und kleine POL-Gruppen mit nur acht Studierenden.
-
Die Betreuung der Studierenden und die Qualität der Lehre ist laut aktuellen Ergebnissen im sogenannten Progress Test Medizin und in den Ärztlichen Prüfungen sehr gut.
-
Die MHB verfügt neben den Universitätskliniken im Verbund über ein großes Netzwerk an weiteren kooperierenden Kliniken und Lehrpraxen. Studierende haben hier während ihres Studiums die Möglichkeit, unterschiedliche klinische Einrichtungen und Fachbereiche intensiv kennenzulernen, was bei der Entscheidung für eine spätere berufliche Fachrichtung sehr hilfreich ist.
-
Last but not least besteht an der MHB die Möglichkeit der Promotion zum Dr. med. in allen Bereichen der medizinischen Forschung. In dem fest ins Studium integrierten Wissenschaftspraktikum kann frühzeitig die erste Grundlage für eine spätere Dissertation gelegt werden.
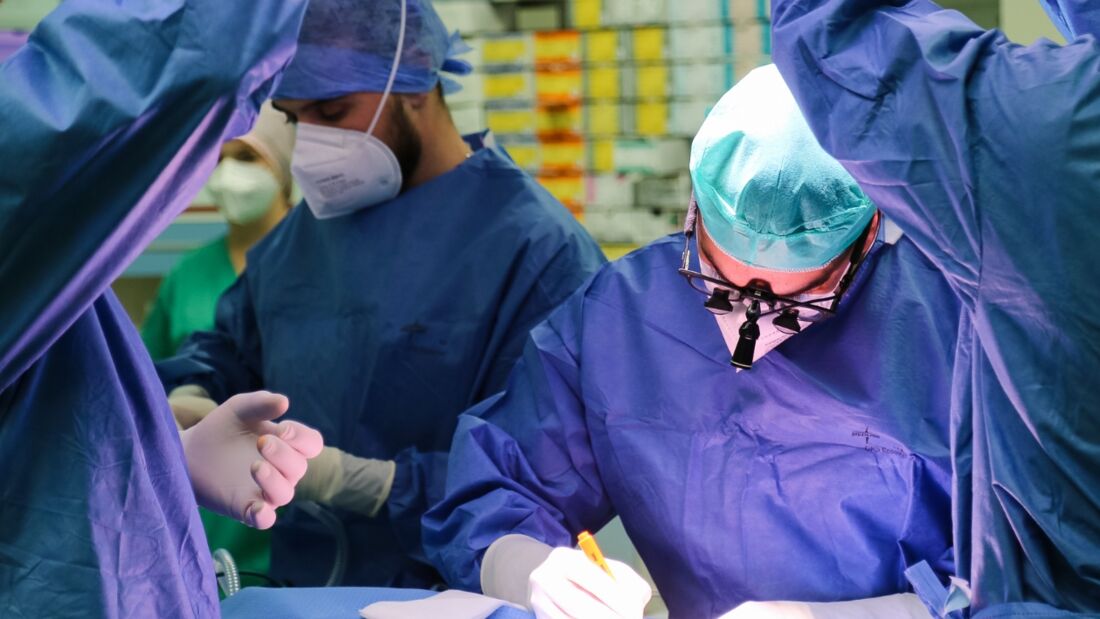
Praxisorientiert &
wissenschaftsbasiert
Der Brandenburgische Modellstudiengang Medizin (BMM) ist seit 2015 staatlich anerkannt und folgt der Modellklausel nach § 41 der Ärztlichen Approbationsordnung (ÄApprO). Gemeinsam mit unseren Universitätskliniken in Bernau, Brandenburg an der Havel, Neuruppin und Rüdersdorf sowie weiteren zahlreichen kooperierenden Kliniken und akademischen Lehrpraxen im Land Brandenburg steht er für ein praxisorientiertes und wissenschaftsbasiertes sowie kompetenzorientiertes und interdisziplinäres Medizinstudium auf höchstem akademischen und medizinischen Niveau.
Das Curriculum ist ausgehend von Lernzielen in verschiedene Module gegliedert.
Der Erste Studienabschnitt (1. - 5. Semester) orientiert sich an Organsystemen des menschlichen Körpers. Hierbei werden aus dem Blickwinkel der grundlagenwissenschaftlichen und klinischen Fachgebiete der gesunde Körper mit seinen Organen, dessen Aufbau, Funktionen und Störungen sowie den daraus resultierenden Erkrankungen und Behandlungsmöglichkeiten betrachtet. Der Erste Abschnitt der Ärztlichen Prüfung („Physikum“) wird im Rahmen von hochschulinternen Äquivalenzprüfungen in den ersten fünf Semestern abgelegt.
Bereits ab dem 2. Semester absolvieren unsere Studierenden Praktika bei niedergelassenen Ärzt*innen im Land Brandenburg. Während der Praxistage haben die Studierenden die Möglichkeit, die ärztlichen Kolleg*innen zu beobachten und erlernte praktische Fähigkeiten unter Supervision anzuwenden.
Im Zweiten Studienabschnitt (6. - 10. Semester) vertiefen die Studierenden ihr Wissen in den verschiedenen klinischen Fachgebieten der Medizin. In den interdisziplinären Modulen bauen die Studierenden ihr klinisches Wissen und ihre praktischen Fertigkeiten im Rahmen einer Lernspirale weiter aus. Unter Beibehaltung der engen Verzahnung von Praxis und Theorie werden in den Universitätskliniken, akademischen Lehrkrankenhäusern und kooperierenden Krankenhäusern strukturierte klinische Praktika angeboten.
Der frühzeitige und intensive Praxiskontakt fördert bei den Studierenden das Verständnis für Zusammenhänge zwischen naturwissenschaftlichen Grundlagen, Krankheitsbildern und dem Krankheitserleben. Darüber hinaus lernen die Studierenden schrittweise die Übernahme von Verantwortung in der Patient*innenversorgung.
Nach dem Abschluss des Zweiten Studienabschnittes legen die Studierenden den Zweiten Abschnitt der Ärztlichen Prüfung ab und absolvieren das Praktische Jahr (PJ).
Darüber hinaus umfasst das Studium einen dreimonatigen Krankenpflegedienst, eine Ausbildung in Erster Hilfe und eine viermonatige Famulatur.

Training ärztlicher Fertigkeiten
Das Studium an der MHB ist problemorientiert und studierendenzentriert ausgerichtet. Die Studierenden übernehmen hierbei eine aktive Rolle im Lernprozess. Die Grundlage hierfür bildet das Problemorientierte Lernen (POL) als zentrales innovatives Lehr- und Lernformat. Ausgehend von konkreten, im Studienverlauf komplexer werdenden Problemstellungen werden naturwissenschaftliche Grundlagen zusammen mit relevanten klinischen Inhalten erarbeitet.
Die Studierenden aktivieren in Kleingruppen anhand von konkreten Problemstellungen Vorwissen, identifizieren Wissenslücken und entwickeln darauf aufbauend Lernziele für die Woche. Die Lernziele werden unter Einbeziehung von Inhalten aus Vorlesungen, Seminaren, Übungen und Fachliteratur bearbeitet und in einer weiteren Gruppensitzung diskutiert und zusammengetragen.
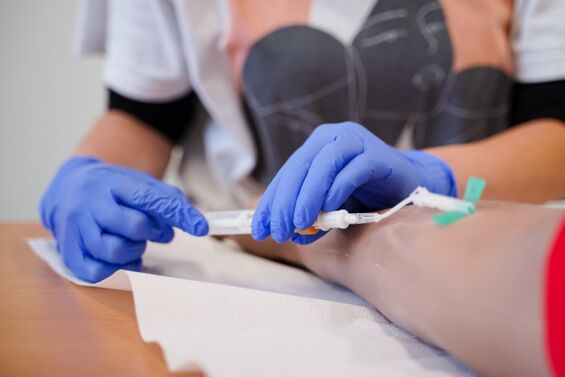
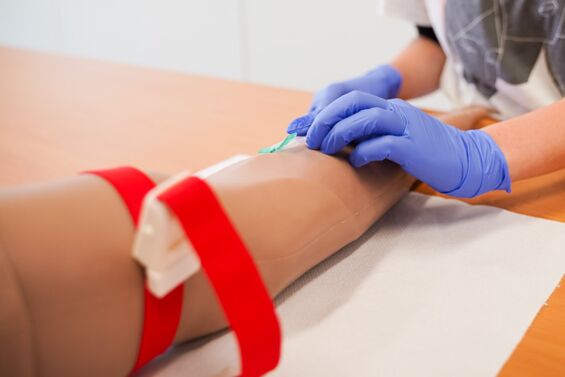
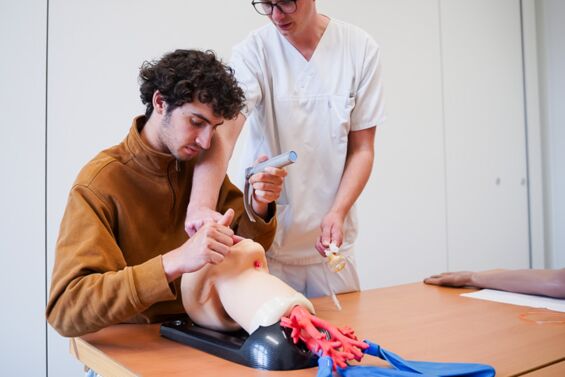
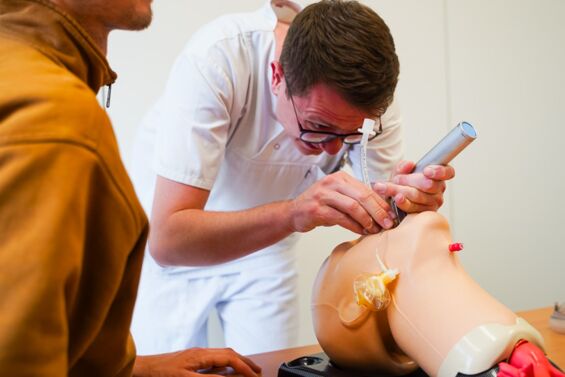
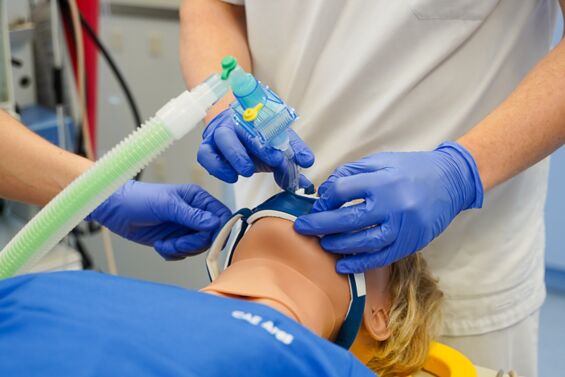
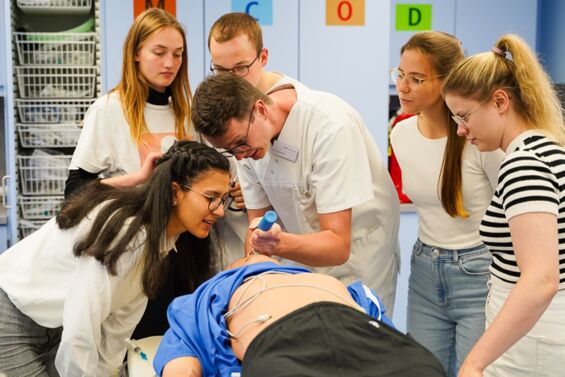
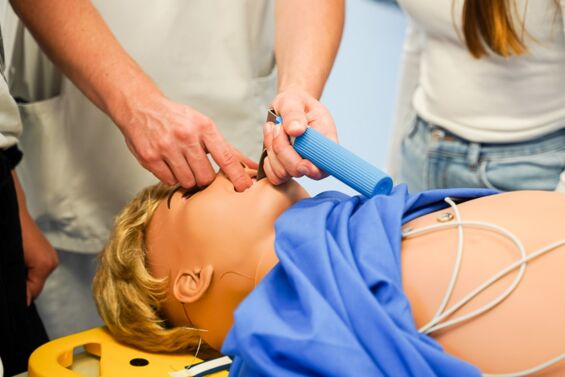
Klinisch-praktische Fertigkeiten werden im Modellstudiengang Medizin ab dem ersten Semester vermittelt und trainiert. Das von der Gesellschaft für medizinischen Ausbildung (GMA) zertifizierte Skills Lab der MHB ist der zentrale Ort für Lehre und Einübung praktischer Fertigkeiten sowie kommunikativer Kompetenzen. Das Skills Lab ermöglicht den Studierenden unter Supervision in einem geschützten Rahmen praktische Fertigkeiten (z.B. Blutentnahme, Ultraschall) zu trainieren. Darüber hinaus können mithilfe von Modellen und Simulatoren Notfallsituationen, Operationen und anderen Szenarien realitätsnah geübt werden. In der Anatomie wird außerdem ein Studium an Körperspender*innen, also an echten menschlichen Präparaten, ermöglicht.
Studium auf einen Blick
Ohne Zulassungsbeschränkung (NC)
Praktisch praxisnah
Studieren auf höchstem akademischen Niveau
TRIK
Ärztliche Tätigkeit ist untrennbar mit kommunikativen Kompetenzen der Gesprächsführung, Teamarbeit und Selbstreflexion verbunden. Über mehrere Semester hinweg werden im Rahmen eines Längsschnittcurriculums für die Übung Teamarbeit, Reflexion, Interaktion und Kommunikation (TRIK) unter enger Anbindung an die fachlichen Inhalte der Module kommunikative Kenntnisse und Fähigkeiten vermittelt.
Durch den Einsatz von Simulationspersonen können Gesprächsführung und herausfordernde Situationen (z.B. Überbringen schlechter Nachrichten) in einem geschützten Rahmen geübt und reflektiert werden. Durch den hohen Stellenwert der Selbstreflexion wird den Studierenden die Möglichkeit gegeben, persönliche Haltungen und Einstellungen weiterzuentwickeln.
Der besonderen Situation im Flächenland Brandenburg Rechnung tragend erhalten Themen wie Versorgungsforschung, Digitalisierung, Telemedizin, Prävention oder Gesundheitswissenschaften ein stärkeres Gewicht und werden in einem eigenen Modul „Gesundheitsversorgung“ fokussiert. Darüber hinaus gibt es ein größeres Angebot frei wählbarer Veranstaltungen z.B. im Bereich „Grundlagen ärztlichen Denken und Handelns“.
Mehr über TRIK aus der Perspektive der Studierenden erfahren Sie hier in dem Video!
Qualität der Lehre
Die Lehre an der MHB findet eingebettet in Forschung und Krankenversorgung statt, wird von qualitätssichernden Maßnahmen wie dem Progress Test Medizin begleitet und durch eine hochwertige und moderne Lehr-Infrastruktur getragen.
Die Qualität der Lehre und der Studienbedingungen an Universitäten ist grundsätzlich nicht einfach zu messen. Ein guter Indikator ist jedoch die Bestehens- und Abschlussquote in Regelstudienzeit: Der überwiegende Teil der Medizinstudierenden der MHB schließt das 2. und 3. Staatsexamen erfolgreich innerhalb der Regelstudienzeit ab. 98% der MHB-Studierenden besteht das zweite Staatsexamen im ersten Versuch. Mit dieser Quote liegt die MHB weit vor allen anderen deutschen Universitäten.
Bei den Ergebnissen der 2. Ärztlichen Prüfung, welche zentral durch das IMPP gestellt und ausgewertet wird, bewegen sich die Studierenden der MHB regelmäßig auf Augenhöhe mit den Studierenden anderer Fakultäten. Bei den Ergebnissen der letzten schriftlichen Examensprüfungen lagen die Studierenden der MHB sogar vor einigen anderen renommierten Medizinischen Fakultäten. Auch wenn die statistischen Unterschiede minimal und für die berufliche Praxis nicht wirklich aussagekräftig sind, so zeigen die Prüfungsergebnisse doch, dass sich die Qualität der Lehre im Brandenburgischen Modellstudiengang Medizin insgesamt auf einem hohen Niveau bewegt. Die detaillierten Ergebnisse des zweiten Staatsexamens finden sich hier.
Progress Test Medizin (PTM)
Die hohe Qualität der Lehre an der MHB wird nicht nur durch diese Prüfungsergebnisse, sondern zuvor schon durch beständige interne Evaluationen und daraus abgeleitete Weiterentwicklungen des Lehrangebots gesichert. Die hier erzielten Erfolge lassen sich auch an der Ergebnissen des regelmäßig durchgeführten Progress Test Medizin (PTM) ablesen. An dem durch die Charité Universitätsmedizin Berlin entwickelten, zusammengestellten und ausgewerteten Test nehmen jährlich rund 10.000 Studierende von 15 Fakultäten aus Deutschland und Österreich teil. Die Studierenden der MHB schneiden auch bei diesem Test regelmäßig überdurchschnittlich ab.
Sehr gutes Betreuungsverhältnis
Ein weiterer wesentlicher Grund für die hohe Qualität der Lehre liegt in der Betreuungsrelation, die abbildet, wie viele Studierende auf eine Professur kommen. Im Bundesdurchschnitt liegt dieses Verhältnis bei 1 zu 65, mit deutlichen regionalen Unterschieden: Thüringen liegt mit einem Verhältnis von 1 zu 43 an der Spitze der Bundesländer, NRW bildet mit einem Verhältnis von 1 zu 90 das Schlusslicht. Mit einer Relation von 1 zu 14 bietet die MHB bundesweit ein herausragendes Betreuungsverhältnis, was auch für eine exzellente Qualität der Lehre und der Studienbedingungen spricht!
1
14
43
65
90
Studienberatung

Frag uns Studierende!
Hello



Samira Dabelow
Studentische Studienberatung
Du hast inhaltliche Fragen zum Studium oder zum Studierendenleben an der MHB? Oder du möchtest dir vor Ort selbst ein Bild machen und studieren probieren? Da kannst du gerne auch unsere studentische Studienberatung kontaktieren. Dort erhältst du authentische Informationen zu Besonderheiten eines Studiums an der MHB direkt aus erster Hand.
Gerne kannst du hier Kontakt aufnehmen und ein persönliches Gespräch vereinbaren. Wir freuen uns auf deine Nachricht!
Wissenswertes
Studienbeginn: 01. April (Sommersemester) und 01. Oktober (Wintersemester)
Studienabschluss: Staatsexamen
Bewerbungsfristen: Bewerbungen sind jederzeit online möglich: Fristende 31. Oktober (Sommersemester) und 30. April (Wintersemester). Die Plätze für die persönlichen Auswahltage werden laufend vergeben, daher empfehlen wir eine möglichst frühzeitige Bewerbung.
Studienplätze: jeweils 69
Regelstudienzeit: 6 Jahre und 3 Monate
Studienorte: Neuruppin, Brandenburg an der Havel, Bernau/Rüdersdorf
Akkreditierung: Staatliche Anerkennung als Modellstudiengang im Sinne der Approbationsordnung für Ärzte (ÄApprO)
Lehrsprache: Deutsch
Studienbeitrag: 118.000 Euro
Zulassungsvoraussetzungen: Hochschulzulassungsberechtigung gemäß BbgHG
Bewerbungsverfahren: Kein NC! Schriftliche Bewerbung und persönliches Auswahlverfahren
Bewerbungsgebühr: 200 Euro pro Bewerbungsverfahren
Weitere Gebühren: derzeit 260 Euro pro Semester (VBB-Semesterticket Berlin-Brandenburg in Höhe von 200 Euro und Sozialbeitrag in Höhe von 60 Euro für studentische Projekte u.ä.)
Persönlichkeit, Motivation und Praxiserfahrungen zählen mehr als Abiturnoten
Unter dem Motto "Persönlichkeit statt NC!" erfolgt die Auswahl der Studierenden nach personalen Kriterien. Motivation, Praxiserfahrung und Persönlichkeit spielen dabei eine größere Rolle als der Notendurchschnitt. Sehr gute Abiturnoten signalisieren zwar Lern- und Leistungsbereitschaft und sind ein guter Indikator für den zu erwartenden Studienerfolg, sie sind aber keine Garantie für eine spätere empathische Tätigkeit als Ärztin oder Arzt. Neben sehr guten Noten benötigen gute Ärzt*innen auch noch andere Stärken und Kompetenzen. Daher legen wir in unserem Auswahlverfahren auf die Persönlichkeit unserer Bewerber*innen einen besonderen Wert.
Medizin studieren ohne Abitur
Laut Brandenburgischem Hochschulgesetz (BbgHG) ist ein Studium der Medizin im Land Brandenburg auch ohne die Allgemeine Hochschulreife (Abitur) möglich. Dementsprechend werden von der MHB neben der Allgemeinen Hochschulreife alternativ auch andere Qualifikationen anerkannt. Hierzu zählen etwa die fachgebundene Hochschulreife, die Fachhochschulreife oder ein erster berufsqualifizierender Hochschulabschluss.
Allerdings ist dabei zu beachten, dass die fachgebundene Hochschulreife und die fachgebundene Fachhochschulreife nur zum Studium in der entsprechenden Fachrichtung berechtigen.
Näheres wird durch das Brandenburgische Hochschulgesetz (BbgHG), Abschnitt 2, § 9 (2), geregelt, das Sie hier finden.
Bei Fragen hierzu können Sie sich gerne auch an die Studienberatung der MHB, Cornelia Gammelin, wenden, die Sie per Telefon unter 03391 39-14210 und per E-Mail unter studienberatung@mhb-fontane.de erreichen.
Regelung für Neuabiturient*innen
Sollten Sie zum Zeitpunkt Ihrer Bewerbung noch kein Abiturzeugnis vorliegen haben, ist eine Bewerbung auch mit dem Nachweis des letzten Halbjahreszeugnisses möglich. Bitte geben Sie in diesem Fall im Rahmen der Online-Bewerbung Ihre aktuelle Durchschnittsnote sowie das Datum des voraussichtlichen Abschlusses an und laden das Halbjahreszeugnis hoch. Das Abiturzeugnis muss spätestens zum Immatrikulation nachgereicht werden.
Sowohl im praxisorientierten Studium als auch individuellen Bewerbungsverfahren spielen Persönlichkeit und Persönlichkeitsentwicklung die zentrale Rolle. Als staatlich anerkannte, aber überwiegend nicht staatlich finanzierte Universität in kommunaler und gemeinnütziger Trägerschaft leistet sich die Medizinische Hochschule Brandenburg ein eigenes, aufwändiges und personalintensives Auswahlverfahren.
Unter dem Motto "Persönlichkeit statt NC!" erfolgt die Auswahl unserer Studierenden nach individuellen Kriterien. Motivation, Praxiserfahrung und Persönlichkeit stehen hierbei im Vordergrund. Einen notenbasierten „Numerus Clausus“ (NC) gibt es hingegen nicht.
1. Schritt: Online-Bewerbung
Ihre Bewerbung für den Modellstudiengang Medizin ist ganzjährig über unsere Online-Bewerbungsmaske möglich. Bitte reichen Sie dafür folgende Unterlagen ein:
1. Detailliertes Motivationsschreiben (höchstens zwei DIN-A4-Seiten, Schriftgröße 11 pt): Was reizt Sie daran Medizin studieren und als Ärzt*in arbeiten zu wollen? Wie sind Sie zu Ihrem Wunsch gekommen, Medizin studieren zu wollen? Welche Erfahrungen/Eindrücke haben Sie dabei geprägt?
2. Bewerbungsfragen (höchstens eine DIN-A4-Seite für beide Fragen zusammen, Schriftgröße 11pt)
Frage 1: Wissenschaftliche Kompetenzen haben für die Tätigkeit als Ärzt*in eine erhebliche Bedeutung. Nehmen Sie zu diesem Zusammenhang ggf. anhand eigener Beobachtungen/Erfahrungen Stellung.
Frage 2: Welche Erwartungen verbinden Sie mit dem Modellstudiengang Medizin an der MHB?
3. Ausführlicher tabellarischer Lebenslauf (ohne Passfoto) - Insbesondere Angaben von Erfahrungen im medizinischen Bereich, besonderen Kenntnissen/Aktivitäten und/oder sozialen Engagement.
4. Hochschulzugangsberechtigung oder Äquivalent
5. Aktuelle Zeugnisse/Beurteilungen (z. B. Ausbildungen, Studienabschlüsse, Empfehlungsschreiben)
6. Internationale Bewerber:innen: Nachweis Deutschkenntnisse (Level C1)
Fügen Sie Ihre vollständigen Bewerbungsunterlagen in der oben genannten Reihenfolge in einer zusammenhängenden pdf-Datei zusammen (bitte keine Umlaute und Sonderzeichen verwenden).
Vorgabe für die Dateibezeichnung: Nachname_Vorname_Bewerbung_Humanmedizin
Bei erfolgreicher Online-Bewerbung erhalten Sie eine automatische Bestätigung per E-Mail. Bitte beachten Sie, dass wir nur vollständig eingereichte Unterlagen berücksichtigen können und eine Nachreichung nicht möglich ist.
2. Schritt: Prüfung und Beurteilung der Unterlagen
Nach Bewerbungseingang werden die Unterlagen auf Vollständigkeit und auf die formalen Zulassungsvoraussetzungen hin geprüft. Anschließend werden diese von unseren Gutachter*innen gelesen und beurteilt. Danach bekommen Sie von uns per E-Mail eine Benachrichtigung, ob wir Sie zu einem der Auswahltage einladen werden oder leider auch nicht. Im Falle einer Absage bitten wir um Ihr Verständnis, dass wir Ihnen die Gründe unserer Entscheidungsfindung nicht mitteilen.
3. Schritt: Persönliche Vorstellung am Auswahltag
Im Rahmen des persönlichen Auswahltages in Neuruppin lernen wir Sie und Sie uns besser kennen. Hierbei durchlaufen Sie mehrere Stationen und treffen auf Fakultätsmitglieder und Studierende, die Sie auch im weiteren Studium begleiten werden. Im Rahmen unseres Auswahlverfahrens wird kein spezifisches fachliches Wissen abgeprüft, vielmehr geht es uns darum, Ihre Motivation, Persönlichkeit und Haltung kennenzulernen. Gleichzeitig haben Sie die Möglichkeit, Fragen zum Studium und zu unserer Universität zu stellen.
Im Anschluss an die Auswahltage erhalten Sie zeitnah von uns eine Rückmeldung per E-Mail. Entweder wird Ihnen ein Studienplatz angeboten oder Sie erhalten einen ablehnenden Bescheid. Wir bitten um Ihr Verständnis, dass wir im Falle einer Absage keine inhaltliche Begründung geben.
Bei Fragen zum Studium oder zum Bewerbungsverfahren wenden Sie sich bitte an:
Bewerbungsbüro Medizin
Tel: +49 (0)3391 39-14210
E-Mail: studienberatung@mhb-fontane.de
Wir wünschen Ihnen viel Erfolg bei Ihrer Bewerbung!
Bitte beachten Sie, dass das Medizinstudium sowohl zum Sommersemester als auch zum Wintersemester startet! Es werden jeweils 69 Studienplätze vergeben.
Bewerbungen sind jederzeit möglich. Die Bewerbungsfrist für einen Studienstart im Sommersemester endet am 31.10., die Bewerbungsfrist für das Wintersemester endet am 30.04. Die Plätze für die persönlichen Auswahltage werden laufend vergeben.
Wenn Sie aktuell bereits Humanmedizin an einer anderen Universität studieren (oder bereits an einer anderen Universität studiert haben), können Sie sich für den Einstieg in ein höheres Fachsemester unseres Modellstudiengangs bewerben. Ein Wechsel an die MHB setzt freie Studienkapazitäten im jeweiligen Jahrgang voraus.
Die Aufnahme von Studierenden ist grundsätzlich in das 5. Fachsemester nach Bestehen bzw. Anrechnung des Ersten Abschnitts der Ärztlichen Prüfung möglich. Sofern Ihr bisheriges Studium im Ausland erfolgte, müssen Sie zur Bewerbung einen Anrechnungsbescheid Ihrer im Ausland erfolgten Studienzeiten und -leistungen durch das zuständige Landesprüfungsamt vorlegen.
Bitte beachten Sie die besonderen Bewerbungsfristen: Wintersemester: 30.06.; Sommersemester: 31.12.
Nehmen Sie bei Fragen gern Kontakt zu uns auf, entweder per E-Mail unter studienberatung@mhb-fontane.de oder per Telefon unter 03391 39-14230.
Die Medizinische Hochschule Brandenburg Theodor Fontane ist eine staatlich anerkannte Universität in kommunaler und gemeinnütziger Trägerschaft. Da sie aktuell zwar staatliche Mittel für den weiteren Ausbau ihres Forschungsbereichs, nicht aber für die in einem Modellstudiengang besonders aufwändige und kostenintensive Lehre erhält, muss sie alle hier anfallenden Kosten mit eigenen Mitteln bewältigen. Neben den Gesellschaftern und Universitätskliniken beteiligen sich auch die Studierenden an den Kosten ihres Studiums, wobei es unser Ziel und Anspruch ist, ein Studium an der MHB nicht an der Frage der Finanzierung scheitern zu lassen.
Jede:r soll studieren können!
Die Studiengebühren für den Brandenburger Modellstudiengang Medizin betragen insgesamt 118.000 Euro. Damit ein Studium an der MHB nicht an der Frage des Geldes scheitert, sondern eine Frage der Persönlichkeit und Eignung bleiben kann, sind bei der Finanzierung des Studiums verschiedene Wege möglich:
1. Studienkredit der Sparkasse Ostprignitz-Ruppin
Studiengebühren, Studienplatzkosten und sogar Lebenshaltungskosten können bequem und flexibel mit dem MHB-Studienkredit unseres Kooperationspartners und Gesellschafters der Sparkasse Ostprignitz-Ruppin finanziert werden. Die Rückzahlung des Kredits beginnt erst nach Abschluss des Studiums.
Weitere Informationen und Beispielrechnungen erhalten Sie hier oder persönlich in der folgende Geschäftsstelle:
|
Mediale Geschäftsstelle |
|
Laura Sauter |
|
Tel.: 03391 81-1366 |
|
E-Mail: gs-medial@sparkasse-opr.de |
2. Brain Capital Bildungsfonds
Brain Capital wurde als Startup an der WHU Otto Beisheim School of Management gegründet und bietet seit mehr als 15 Jahren Studierenden eine innovative Finanzierungslösung für Studiengebühren. Anders als bei einem Studienkredit, der in der Regel zur zeitnahen Rückzahlung auffordert, bieten Brain Capital Bildungsfonds eine einkommensabhängige, nachgelagerte Rückzahlung. Derzeit gibt es 33 Partnerhochschulen und über 9.500 Förderverträge.
Brain Capital übernimmt dabei anteilig die direkte Zahlung der fälligen Studiengebühren an die Hochschule. Es gibt keine Tilgung oder Zinszahlung während der Studienzeit. Stattdessen zahlen die ehemaligen Studierenden nach erfolgreichem Abschluss des Studiums und einem Mindesteinkommen von 30.000 Euro brutto pro Kalenderjahr einen festen Prozentsatz ihres Einkommens für 12 Zahlungsjahre. Liegt das Einkommen unter dem Mindesteinkommen, fällt in diesem Jahr keine Rückzahlung an. 20 Jahre nach Studienabschluss endet die Zahlungsverpflichtung, unabhängig von den tatsächlich geleisteten Zahlungen und Zahlungsjahren. Die Rückzahlungssumme ist auf das Doppelte der Fördersumme (inflationsbereinigt) begrenzt.
Weitere Details finden Sie hier.
3. Studienfonds der Deutschen Bildung
Eine andere Möglichkeit, das Studium zu finanzieren, ist der Weg über den Studienfonds der Deutschen Bildung.
Unabhängig vom Einkommen der Eltern erhalten Studierende eine Restfinanzierung, die Sie ohne fixe Schuldenlast ebenfalls im Sinne eines Umgekehrten Generationenvertrags zurückzahlen: Erst nach Einstieg in den Beruf zahlen Sie einen festgelegten Prozentsatz Ihres Bruttoeinkommens über einen festen Zeitraum zurück – immer an Ihre individuelle Arbeits- und Lebenssituation angepasst.
Weitere Informationen zur Deutschen Bildung finden Sie hier, hier geht es direkt zur Online-Bewerbung.
4. Studienförderung durch eine kooperierende Klinik der MHB
Die Gründung der MHB erfolgte vor dem Hintergrund der auch in ländlichen Regionen dringend benötigten Ärzt*innen. Im Sinne der Nachwuchsförderung haben sich kooperierende Kliniken der MHB entschieden, sich mit 80.000 Euro an den Studiengebühren einzelner Studierender zu beteiligen.
Mit einem solchen Klinikstipendium ist eine vertragliche Regelung zwischen dem/der jeweiligen Studierenden und dem Krankenhaus verbunden. Diese Vereinbarung sieht im Anschluss an das Studium eine fünfjährige ärztliche Tätigkeit in diesem Krankenhaus vor. Gleichzeitig verpflichtet sich das Krankenhaus, bei voller tariflicher Bezahlung die Absolvierung der kompletten Weiterbildung in den jeweilig angebotenen Fachgebieten zu ermöglichen.
Grundsätzlich kann ein Klinikstipendium über zwei Wege vergeben werden:
1. Vor der Bewerbung und einer Studienplatzzusage durch die MHB: Empfehlung einer kooperierenden Klinik
Bewerber:innen, welche bereits vor Studienbeginn einen persönlichen und engen Bezug (z.B. durch eine Ausbildung) zu einer unserer kooperierenden Kliniken haben, können sich bereits vor der Bewerbung und einer möglichen Studienplatzzusage durch die MHB bei der jeweiligen Klinik um ein Klinikstipendium bewerben. Sollte Ihnen die Klinik ein Stipendium anbieten, werden Sie direkt zu einem der Auswahltage eingeladen und nehmen dann am regulären Auswahlverfahren der MHB teil.
Bitte beachten Sie, dass Sie sich dementsprechend mit allen erforderlichen Unterlagen online fristgerecht bei uns bewerben müssen. Bitte beachten Sie ebenfalls, dass die Bewerbung um ein Klinikstipendium sinnvollerweise nur an einer und nicht an mehreren kooperierenden Kliniken möglich ist. Bei Interesse an einem Klinikstipendium und bei weiteren Fragen zum jeweiligen Bewerbungsverfahren wenden Sie sich bitte direkt an die kooperierende Klinik Ihrer Wahl.
2. Nach Studienplatzzusage durch die MHB
Ziel ist es, eine bestmögliche Passung zwischen den Wünschen und Vorstellungen unserer Studierenden auf der einen Seite und den fachärztlichen Weiterbildungsangeboten unserer kooperierenden Kliniken auf der anderen Seite herzustellen. Hierbei sind auch flexible Lösungen möglich, bei der sowohl die Höhe der Stipendien als auch die Dauer der vereinbarten Weiterbildung variieren können. So lassen sich die individuellen Weiterbildungsbefugnisse eines Hauses noch besser mit den individuellen Weiterbildungswünschen der Studierenden abstimmen. Medizinstudierende können sich so auch noch während des Studiums direkt bei einer kooperierenden Klinik um ein Stipendium mit anschließender fachärztlicher Weiterbildung bewerben.
Auch wenn wir uns als MHB kontinuierlich um die weitere Steigerung der zu vergebenden Klinikstipendien bemühen, steht dennoch leider nur eine begrenzte Anzahl an Klinikstipendien zur Verfügung. Dementsprechend weisen wir darauf hin, dass leider nicht alle interessierten Studierenden ein Stipendium erhalten können. Bitte informieren Sie sich daher bereits frühzeitig auch über alternative Finanzierungsmöglichkeiten.
Tipp: Auch jenseits der Finanzierung der Studienbeiträge durch ein Stipendium einer unserer kooperierenden Kliniken haben Sie natürlich die Möglichkeit, auch mit einer anderen Klinik Ihrer Wahl, die Sie vielleicht schon kennt und in der Sie womöglich eine Ausbildung oder ein Praktikum im Krankenpflegedienst absolviert haben, eine individuelle Vereinbarung zu treffen, welche die Finanzierung Ihres Studiums an der MHB mit einer späteren Berufstätigkeit an dieser Klinik verbindet.
5. Eigenfinanzierung
Unabhängig von diesen genannten Optionen besteht natürlich auch die Möglichkeit, die Studienbeiträge vollständig mit eigenen Mitteln zu finanzieren.
Neben den Studienbeiträgen fallen für ein Studium grundsätzlich Lebenshaltungskosten an. Auch hier gibt es eine Vielzahl verschiedener Finanzierungsmöglichkeiten, von denen wir Ihnen beispielhaft einige nennen wollen:
1. Studienkredit der Sparkasse Ostprignitz-Ruppin
Studiengebühren, Studienplatzkosten und sogar Lebenshaltungskosten können bequem und flexibel mit dem MHB-Studienkredit unseres Kooperationspartners und Gesellschafters der Sparkasse Ostprignitz-Ruppin finanziert werden. Weitere Informationen und Beispielrechnungen erhalten Sie hier oder persönlich in der folgenden Geschäftsstelle:
|
Mediale Geschäftsstelle |
|
Laura Sauter |
|
Tel.: 03391 81-1366 |
|
E-Mail: gs-medial@sparkasse-opr.de |
2. BAföG
Studierende der MHB haben grundsätzlich Anspruch auf Leistungen nach dem Bundesausbildungsförderungsgesetz. Die Förderung ist jedoch an eine Reihe von Bedingungen geknüpft.
Ausführliche Informationen finden Sie hier oder hier.
Weitere Details und Fragen beantwortet Ihnen: Studentenwerk Potsdam, Amt für Ausbildungsförderung, Postfach 01353, Besucheradresse: Babelsberger Str. 2, 14473 Potsdam, Tel.: 0331 3706–0.
3. Teilstudiendarlehen des ukrb
Die Klinik für Psychiatrie, Psychotherapie und Psychosomatik am Universitätsklinikum Ruppin-Brandenburg (ukrb) unter der Leitung von Prof. Joachim Behr bietet ein Teilstudiendarlehen an. Die Höhe des Darlehens richtet sich nach den an der Klinik absolvierten Weiterbildungs- bzw. Beschäftigungszeiten. Wie beim regulären Klinikdarlehen wandelt sich das Teilstudiendarlehen in Abhängigkeit von der Dauer der späteren Beschäftigung in ein nicht zurückzuzahlendes Stipendium.
Interessierte anderer Fachrichtungen können sich zudem in der Regel ein Jahr der Weiterbildungszeit an der Klinik für Psychiatrie, Psychotherapie und Psychosomatik für ihre jeweilige Facharztweiterbildung anrechnen lassen. Neben der klinischen Ausbildung besteht die Möglichkeit der berufsbegleitenden Promotion mit Freistellungszeiten. Bewerben können sich Medizinstudierende ab dem 9. Semester sowie Absolvent:innen des Studiengangs Medizin der MHB. Weiterführende Informationen und die genauen Bewerbungsmodalitäten entnehmen Sie bitte diesem Dokument.
4. Stipendium der Stadt Wittenberge für Medizin-Studierende
Wer Mediziner:in werden und später in einer charmanten Stadt leben und arbeiten möchte, kann sich um ein medizinisches Stipendium der Stadt Wittenberge (Prignitz) bewerben. Das Stipendium bietet eine monatliche Unterstützung von 700 Euro für einen Zeitraum von maximal 75 Monaten. Im Gegenzug verpflichtet man sich, nach Abschluss der Facharztausbildung fünf Jahre lang in Wittenberge oder den angrenzenden Ortsteilen zu arbeiten. Weitere Informationen dazu sowie zur Bewerbung gibt es auf der Website der Stadt Wittenberge.
5. Deutschlandstipendium
Mit dem Deutschlandstipendium werden engagierte und befähigte Studierende gefördert, „die aufgrund ihres bisherigen Engagements und Werdegangs unter Berücksichtigung sozialer, familiärer und persönlicher Umstände über ein großes Potenzial verfügen und herausragende Leistungen in Studium oder Beruf erwarten lassen oder bereits erbracht haben". Der dem Stipendium zugrundeliegende Leistungsbegriff ist dabei bewusst weit gefasst: Gute Noten und Studienleistungen gehören ebenso dazu wie die Bereitschaft, gesellschaftliche Verantwortung zu übernehmen oder Hindernisse und Widerstände im eigenen Lebens- und Bildungsweg erfolgreich zu meistern.
Die Höhe des Deutschlandstipendiums beträgt 300 Euro pro Monat. Die Stipendiat*innnen erhalten die Förderung in der Regel für mindestens 12 Monate (ein Studienjahr).
Wie viele Stipendien die MHB vergeben kann, hängt dabei zum einen davon ab, wie viele private Fördergelder wir einwerben können, zum anderen auch von der Anzahl der eingeschriebenen Studierenden an der MHB.
Weitere Informationen zum Deutschlandstipendium sowie zu weiteren Fördermöglichkeiten für ein Studium an der MHB finden Sie hier.
6. Studienfonds der Deutschen Bildung
Eine weitere Möglichkeit, das Studium zu finanzieren, ist der Weg über den Studienfonds der Deutschen Bildung.
Unabhängig vom Einkommen der Eltern erhalten Studierende eine Restfinanzierung, die ohne fixe Schuldenlast ebenfalls im Sinne eines umgekehrten Generationenvertrags zurückzahlen ist: Erst nach Einstieg in den Beruf ist ein festgelegter Prozentsatz des Bruttoeinkommens über einen festen Zeitraum zurückzuzahlen – immer an die individuelle Arbeits- und Lebenssituation angepasst.
Weitere Informationen zur Deutschen Bildung finden Sie hier, hier geht es direkt zur Online-Bewerbung.
7. Individuell passende Stipendien
Die Plattform mystipendium.de unterstützt Studierende bei der Recherche nach geeigneten, zum individuellen Lebenslauf passenden Stipendien. Um dies zu ermöglichen, wurden die Bewerbungsvoraussetzungen jeder Förderung in einer Datenbank detailliert erfasst. Sie müssen hier nur noch Ihr Profil anlegen. Anschließend erhalten Sie eine Liste mit Stipendien, die auf Ihren Lebenslauf passen. Für jedes Stipendium werden zudem Ihre individuellen Erfolgsaussichten angegeben. Bislang sind rund 2100 Einträge erfasst, regelmäßig werden weitere Angebote hinzugefügt.
Hier geht’s zur Homepage von mystipendium.de.
8. Landesförderprogramm zur Stärkung der landärztlichen Versorgung
Das Landesförderprogramm für Medizinstudierende und Ärzt*innen in Weiterbildung geht in die nächste Runde. Ab sofort können bis zum 30.08. die Förderanträge für Stipendien für einen Studienstart im Wintersemester gestellt werden!
Im Rahmen der neuen Richtlinie können für 2023 und 2024 jeweils 18 Stipendien zum Wintersemester neu vergeben werden. Es können sich auch höhere Semester bewerben. Dafür verpflichten Sie sich u. a. zu einer mindestens fünfjährigen ärztlichen Tätigkeit nach Abschluss der Facharztweiterbildung in den Fachrichtungen
- Allgemeinmedizin
- Augenheilkunde
- Frauenheilkunde und Geburtshilfe
- Hals-Nasen-Ohrenheilkunde
- Haut- und Geschlechtskrankheiten
- Kinder- und Jugendmedizin
- Kinder- und Jugendpsychiatrie und –psychotherapie
- Neurologie
- Nervenheilkunde oder
- Psychiatrie und Psychotherapie
in der ambulanten Versorgung in ländlichen Regionen* Brandenburgs.
Detaillierte Informationen zum Landesförderprogramm sowie die Antragsunterlagen finden Sie auch auf der Website der KV Brandenburg unter Landärztestipendium.
Informationen zu weiteren Fördermöglichkeiten der KV Brandenburg (Praxistage, Famulatur, PJ) finden Sie hier.
Bei Fragen zum Studium oder zum Bewerbungsverfahren wenden Sie sich bitte an:
Bewerbungsbüro Medizin
Cornelia Gammelin
Tel: 03391 39-14210
E-Mail: studienberatung@mhb-fontane.de
Postanschrift:
Medizinische Hochschule Brandenburg Theodor Fontane
Bewerbungsbüro
Fehrbelliner Str. 38
16816 Neuruppin
Studentische Studienberatung
Sie haben inhaltliche Fragen zum Studium oder zum Student*innenleben an der MHB? Oder Sie möchten sich vor Ort selbst ein Bild machen? Gerne können Sie auch unsere studentische Studienberatung kontaktieren, dort erhalten Sie Informationen direkt aus erster Hand. Weiterhin ist es auch möglich einen Telefontermin für ein persönliches Gespräch zu vereinbaren. Wir freuen uns auf Ihre E-Mail!
E-Mail: frag.uns.med@mhb-fontane.de
Hier finden Sie für den Brandenburger Modellstudiengang Medizin (BMM) die Studienordnung und die Prüfungsordnung zum Download.
FAQ
Die Medizinische Hochschule Brandenburg (MHB) bietet ein Medizinstudium, das sich im hohen Maße an der klinischen Praxis und an Patient*innen orientiert. Die Auswahl der Studierenden erfolgt dabei nicht nach einem notenbasierten NC, sondern nach persönlicher Eignung und beruflicher Vorerfahrung. Ein Medizinstudium an der MHB unterscheidet sich in folgenden wesentlichen Punkten von dem an anderen Hochschulen:
-
Im Unterschied zu anderen, privaten medizinischen Hochschulen verfügt die MHB über ein Universitätsklinikum im Verbund und ermöglicht ihren Studierenden damit ein vollwertiges Medizinstudium auf höchstem medizinischen und akademischen Niveau, inklusive Promotions- und Habilitationsrecht.
-
Die konventionelle Trennung in Vorklinik und Klinik im Regelstudiengang ist im Modellstudiengang an der MHB zugunsten eines integrierten und praxisorientierten Curriculums aufgehoben. Für die Studierenden hat das den unschätzbaren Vorteil, dass die theoretischen Grundlagen in Biologie, Chemie und Physik immer streng auf die klinische Praxis und den individuellen Fall bezogen werden, wodurch das Lernen sehr viel leichter fällt als in herkömmlichen Regelstudiengängen.
-
Im Modellstudiengang an der MHB gibt es dementsprechend kein separates Physikum, anders als bei anderen Medizinischen Hochschulen besteht an der MHB somit auch kein Risiko, an dieser Hürde zu scheitern. Insgesamt ist die Abschluss- und Bestehensquote in Regelstudienzeit an der MHB herausragend hoch.
-
Es gibt vom ersten Semester an einen hohen Praxisanteil und kleine POL-Gruppen mit nur acht Studierenden, die Betreuung der Studierenden und die Qualität der Lehre ist laut aktuellen Ergebnissen im sogenannten Progress Test Medizin und in den ärztlichen Prüfungen sehr gut.
-
Die MHB verfügt neben den Universitätskliniken im Verbund über ein großes Netzwerk an weiteren kooperierenden Kliniken und Lehrpraxen, Studierende haben hier die Möglichkeit, unterschiedliche klinische Einrichtungen und Fachbereiche intensiv kennenzulernen, was bei der Entscheidung für eine spätere Fachrichtung sehr hilfreich ist.
Alle Bewerber*innen für ein Medizinstudium an der MHB haben die gleiche Chance auf einen Studienplatz. Die Abiturnote gilt generell als ein guter Indikator für Leistungsfähigkeit, sagt allerdings nur sehr wenig über die Neigung zur ärztlichen Tätigkeit aus. Motivation, Praxiserfahrung und Persönlichkeit spielen deshalb im Auswahlverfahren eine größere Rolle als der Notendurchschnitt.
Sie können sich auch ohne den Nachweis der Allgemeinen Hochschulreife bewerben, beispielsweise mit fachgebundener Hochschulreife, Fachhochschulreife oder einem berufsqualifizierenden Hochschulabschluss. Näheres wird durch das Brandenburgische Hochschulgesetz (BbgHG) Abschnitt 2, § 9 (2), geregelt, das Sie hier finden.
Ihre Bewerbung für den Brandenburger Modellstudiengang Medizin erfolgt über unsere Online-Bewerbungsmaske. Nach erfolgreicher Online-Bewerbung erhalten Sie eine automatische Bestätigung per E-Mail. Bitte beachten Sie, dass wir nur vollständig eingereichte Unterlagen berücksichtigen können und eine Nachreichung nicht möglich ist.
Mithilfe des Motivationsschreibens möchten wir mehr über Ihre Persönlichkeit und Ihren Werdegang erfahren. Verzichten Sie bitte beispielsweise auf eine Absenderadresse, Empfängerdaten oder eine direkte Ansprache einer Kontaktperson. Es ist ausreichend, in der Kopfzeile des Motivationsschreibens Ihren Vor- und Nachnamen zu nennen.
Bewerbungen sind jederzeit möglich. Die Bewerbungsfrist für einen Studienstart im Sommersemester endet immer am 31.10. des Vorjahres, die Bewerbungsfrist für das Wintersemester endet am 30.04. Die Plätze für die persönlichen Auswahltage werden laufend vergeben.
Die Bewerbungsgebühr beträgt 200 Euro und wird direkt im Rahmen der Online-Bewerbung beglichen. Im Falle einer Stornierung oder Ablehnung Ihrer Bewerbung wird die Bearbeitungsgebühr nicht erstattet. Es besteht auch die Möglichkeit zum Erlass der Bewerbungsgebühr (nähere Informationen finden Sie hier).
Zum Wintersemester ist eine Bewerbung mit Halbjahreszeugnis möglich. Die Teilnahme am Auswahlverfahren erfolgt unter Vorbehalt des Erwerbs der Hochschulzulassungsberechtigung.
Nein.
Ab dem Wintersemester 2022/23 dürfen Sie sich maximal dreimal für den BMM bewerben. Hierbei spielt es keine Rolle, ob Sie bei einem der Versuche zu einem Auswahltag eingeladen wurden oder nicht.
Der TMS hat keinen Einfluss auf das Bewerbungsverfahren.
Das Medizinstudium an der MHB schließt wie bei allen anderen staatlich anerkannten Medizinstudiengängen in Deutschland nach dem Praktischen Jahr (PJ) mit der Dritten Ärztlichen Prüfung (M3) ab. Nach erfolgreichem Abschluss des Studiums kann die Approbation beantragt werden.
Die Studiengebühren belaufen sich auf 118.000 Euro. Die Gebühren werden semesterweise verteilt auf zehn Semester berechnet. Stipendien- und Darlehensangebote sollen dafür sorgen, dass ein Studium nicht an der Frage der Finanzierung scheitert. Wir haben hier in einem Video die Finanzierungsmöglichkeiten zusammengefasst.
Weitere Gebühren: derzeit 260 Euro pro Semester (d. h. VBB-Semesterticket Berlin-Brandenburg in Höhe von derzeit 200 Euro und Sozialbeitrag in Höhe von 60 Euro).
Wir empfehlen, die Studiengebühren mit Hilfe eines Studienkredits der Sparkasse Ostprignitz-Ruppin oder unter Inanspruchnahme eines Umgekehrten Generationenvertrags zu finanzieren. Bewerber*innen, die nach Abschluss ihres Medizinstudiums anschließend bei einer unserer kooperierenden Kliniken die fachärztliche Weiterbildung absolvieren, haben die Möglichkeit, ein Klinikstipendium in Höhe von 80.000 Euro zu erhalten.
Auch bei der Finanzierung der Lebenshaltungskosten empfehlen wir den Studienkredit der Sparkasse Ostprignitz-Ruppin. Die MHB vergibt jährlich eine große Anzahl an Deutschlandstipendien und vergibt auch eigene MHB-Stipendien.
-
Nachweis von Deutschkenntnissen auf C1-Niveau
-
Beglaubigung und Übersetzung der Urkunden
- Hochschulzugangsberechtigungen, die im Ausland erworben wurden, müssen vorab durch das Schulamt Cottbus (Zeugnisanerkennungsstelle) anerkannt werden. Bitte planen Sie entsprechende Bearbeitungszeiten für diesen Schritt rechtzeitig vor den Bewerbungsfristen ein.
Sie können sich bei Fragen zum Studium, zum Bewerbungsgespräch und studentischen Anliegen gern per E-Mail bei Medizinstudierenden melden: frag.uns.med@mhb-fontane.de.